As a healthcare provider and bariatrics surgeon, you are dedicated to ensuring a high success rate for your patient’s weight loss surgery. Patient engagement is critical to how successful your bariatric patient’s results will be. Ensuring their successful results through patient enablement will improve the operational outcomes for your practice as well.
Connecting with your bariatric patient’s intellectual, emotional, and motivational drivers will greatly increase the success rate of your patients after surgical procedures. Communication with your patient to address all of these drivers is a crucial component in this process.
Key Takeaways:
- Patient-doctor communication is crucial to a bariatric patient’s journey.
- Bariatric surgery success rates involve several factors including long-term behavioral modification strategies, intensive pre-surgical dietary adjustment, and post-surgical follow-ups.
- Patient engagement involves connecting with a bariatric patient’s intellect, emotions, and motivations via educational tools and post-surgical consultations to help amplify success rates.
The Importance of Bariatrics Patient Enablement
“Enablement” denotes a process for patients to engage in self-management throughout the entirety of their journey, allowing for improved success.

The concept of patient enablement correlates with preparation, which correlates with successful surgery outcomes. When you aid your bariatric patient with developing their skills, knowledge, and confidence in their health-related decisions, their success rate increases.
Patient enablement via consultations and post-surgery communication is an effective way to improve success rates for bariatric patients after their surgery. Consistent, clear, and constant communication throughout the surgery process, from referral through recovery, is vital for the success of the patient. Such communication is, therefore:
- important during consultations,
- between appointments,
- while your patient self-monitors their progress,
- and as they adjust their dietary requirements.
For instance, follow-up consultations promote personal responsibility and motivation for patients as they cope with post-surgery challenges and adaptations.
Patient enablement studies have revealed the factors involved in how your bariatric patient will experience their clinical outcomes. Some factors include:
- Your patient’s ethnic background. The cultural sensitivity of everyone around them makes a significant difference in their success rate.
- The amount of time you spend in consultation. Focused time in the consultation will create higher levels of trust.
- Involving your patient in your healthcare decision-making process.
- Doctor-patient communication and the creation of positive perceptions. Your communication skills and use of patient-friendly language and medical terminology help bridge the doctor-patient bridge. The result will be increased enablement and satisfaction.
- The quality and continuity of care are positively associated with patient enablement.
The Importance of Patient Engagement in Bariatrics
Patient engagement involves shaping and nurturing your patient-doctor relationship in your healthcare environment. Patient engagement continues to be identified and increasingly recognized as an integral part of healthcare.
A Bariatrics Patient study conducted in 2017 gathered data from study participants to explore and describe the health support needs they require in publicly or privately funded bariatric surgery procedures. Some of the support needs listed included:
- Healthcare professionals, including dieticians, general practitioners, psychologists
- Significant others
- Family members
- Friends
- Fellow bariatric surgery recipients
- Their communities
The study aimed to highlight the importance of support in mediating outcomes of bariatric surgery. The following top factors were viewed by bariatric patients as the most important. The most overlooked, ignored, or inadequately provided to them, however, during their bariatric procedures and aftercare included:
- Psychological support. Bariatric patients place a high emphasis on psychological support as the most important, yet most ignored support, for their health improvement success. Bariatric patients felt psychological support was more important than dietetic support.
- Informative Content. The bariatric patients specifically requested medically-related information through a mix of electronic and non-electronic media. Bariatric surgeon support is crucial, particularly in the area of communication and providing access to comprehensible information that answers your patient’s questions.
Additional theories on the psychosocial dimension of patient engagement continue to be developed.
9 Ways to Connect & Engage with Bariatric Patients
Healthcare providers are just as important as policymakers when it comes to providing accurate, up-to-date health information. This ensures that patients and their support groups can easilyaccess and share appropriate, current information while on the bariatric journey improvement process.
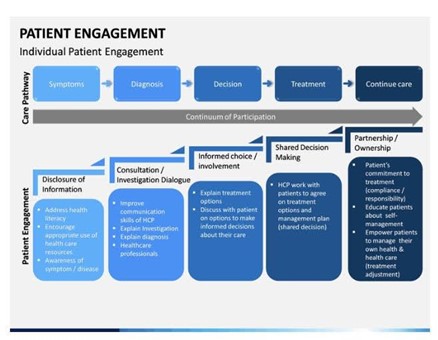
Effective patient engagement starts with the empowerment of bariatric patients.
Providing your bariatric patients with a strong, overall support group and sufficient information about their health and surgical procedures enables your patient to become a knowledgeable partner in decision-making.
Networking and communication remain key components in the health pipeline when motivating a bariatric patient towards success. The health pipeline includes:
- Connecting with Bariatric Patient Support Groups and Sub-communities.
Encourage your patient to access web-based Forums and Online Communities that encourage and support peer-to-peer communication through shared experiences and positive feedback.
- Broader Technological Communication.
Explore and broaden the way you communicate with your patients such as with telephone access, e-mail, and online video calls.
- Patient Apps & Cloud-Based Interactions.
Supply your bariatric patient with your healthcare provider cloud based solution that adapts to any device, or provide them your patient app.
- Access to Electronic Health Records.
Grant bariatric patients access to their own electronic health records. The World Health Organization states that “patient-held records may support the engagement and empowerment of patients”.
- Feedback Systems.
Encourage your bariatric patients to access the feedback systems you provide. Make sure you have feedback systems which your patients prefer. Putting them through a single feedback mechanism will reduce the amount of feedback you receive.
- Educational Materials.
Provide leaflets, PDFs, videos, and other educational materials to your patients.
- Language and Technical Jargon Awareness.
Become aware of your professional or expert language or technical jargon that may create barriers in communication between you and your bariatric patient.
- Cultural and Social Barriers.
Be aware of the cultural and social norms and their impact on the patient engagement process.
- Wellness and Fitness Apps.
Encourage your bariatric patient to access Wellness and Fitness Apps that aid them with tracking their daily food intake and log exercise time.
Other Considerations for Bariatric Patients
The World Health Organization (WHO) has a list of strategies that enhance patient engagement. These include but are not limited to:
- Providing bariatric patients with information on patient-led voluntary associations.
- Identifying and acknowledging the local social and cultural environments constructed by your patients’ socialpatient’s social groups, families, and communities to tap into the positive impact, force and influences they have on your patient.
- Identify and access further human resources, such as advocates, when appropriate to make communication and understanding more accessible and encourage patient engagement
- Implementing mechanisms that support patient engagement at an all systems level.
Apply Modern Tools for Patient Engagement and a Better Road to Recovery
The bariatric market is growing. You and your bariatric patients can tip the scales in your favor by effectively engaging in positive patient-doctor relationships that includes a pipeline of extended support groups, information, and technological measures.
See how Wellbe’s Automated Patient Enablement platform can help the growth of your medical practice. To learn more about our services at WellbBe, please contact us at 1-800-960-4118 or email us.


 The epitome of an entrepreneur, Mark has seen the peaks and valleys of starting, operating, and assuming the risks of a new venture. He’s come up against payroll, had a few bad hires, and even swept the floors early on. Collectively, Mark’s companies have done over $360 million in sales and raised more than $38 million in venture capital, and he has successfully bought and/or sold eight companies.
The epitome of an entrepreneur, Mark has seen the peaks and valleys of starting, operating, and assuming the risks of a new venture. He’s come up against payroll, had a few bad hires, and even swept the floors early on. Collectively, Mark’s companies have done over $360 million in sales and raised more than $38 million in venture capital, and he has successfully bought and/or sold eight companies. James believes technology, when creatively applied, can improve our life experiences. Intrigued by the amazing potential for internet and mobile technology to engage us all, James created a business model to reshape personal health management.
James believes technology, when creatively applied, can improve our life experiences. Intrigued by the amazing potential for internet and mobile technology to engage us all, James created a business model to reshape personal health management. Mike Splinter, an electrical engineer and innovator, has played a major role in driving advances in the high tech industry, with more than four decades of executive leadership experience including 12 years with Applied Materials, Inc. where he was served as chairman and CEO, and over 20 years with Intel, where he was executive vice president of sales and marketing, and executive vice president of the Technology and Manufacturing Group.
Mike Splinter, an electrical engineer and innovator, has played a major role in driving advances in the high tech industry, with more than four decades of executive leadership experience including 12 years with Applied Materials, Inc. where he was served as chairman and CEO, and over 20 years with Intel, where he was executive vice president of sales and marketing, and executive vice president of the Technology and Manufacturing Group. Mr. Baldwin was most recently Chairman and CEO of Baxa Corporation, a leader in devices, systems, and software for the handling, packaging, and tracking of fluid medications in a critical care setting. Under his leadership from 1997 until its sale to Baxter Corporation in 2011, the company sales grew from $25 million to over $170 million. As CEO, he led the eight-member board of directors and led a minority recap resulting in Goldman Sach’s private equity group owning 27% of the company. He was also an early investor and lead director in Pharmacy OneSource, an innovative software-as-a-service business that had a successful exit in 2010.
Mr. Baldwin was most recently Chairman and CEO of Baxa Corporation, a leader in devices, systems, and software for the handling, packaging, and tracking of fluid medications in a critical care setting. Under his leadership from 1997 until its sale to Baxter Corporation in 2011, the company sales grew from $25 million to over $170 million. As CEO, he led the eight-member board of directors and led a minority recap resulting in Goldman Sach’s private equity group owning 27% of the company. He was also an early investor and lead director in Pharmacy OneSource, an innovative software-as-a-service business that had a successful exit in 2010.